
How well the vagus nerve functions is a strong determinant of health; vagus nerve dysfunction is highly associated with disease. – Dr. Navaz Habib
As I’m typing the word ‘vagus’ for the draft copy of this post, MS Word underlines it, indicating that it’s not in the program’s vocabulary. And I could hear my brain saying, “ditto,” hah! I bet yours, too.
While it’s understandable for common people like us not to memorize our body’s anatomy since our organs do their respective jobs pretty well without our knowing, there’s this one part of our bodily systems that cannot be overlooked anymore — the vagus nerve.
I wonder why it was never even mentioned in our biology class and never written about in science books.
Thanks to Dr. Navaz Habib’s book, Activate Your Vagus Nerve, I learned and understood — and hopefully by the end of this article, you will as well – the key significant role the vagus nerve plays to keep us alive.
Nope, I’m not exaggerating. Ever wondered how our hearts are able to beat and we’re able to breathe involuntarily? That’s the vagus nerve in action!
The vagus nerve takes care of everything happening inside our bodies so we no longer have to think about them and we can go on living our lives.
Now, how about we take some time out of our busy schedules to give it back our care and attention?
Vagus nerve awesomeness, activated!
What and Where is the Vagus Nerve
The vagus nerve (actually the vagus nerves, as there are two paired structures, with one present on each side of the body) is responsible for regulating control of the heart, lungs, muscles of the throat and airway, liver, stomach, pancreas, gallbladder, spleen, kidneys, small intestine, and part of the large intestine.
The vagus nerve is the single most important communication pathway regarding digestion, nutrient status, and the ever-changing population of bacteria, viruses, yeast, parasites, and worms that live within our digestive tracts.
Vagus comes from a Latin word meaning “wanderer.” Why? Because its functions go all throughout the body, anatomists wanted a descriptive term as such.
The vagus nerve is the longest nerve in the body and it’s the only nerve that originates from the brainstem (the trunk of the brain that senses, processes, and regulates the automatic functions of the body) and runs through the entire body.
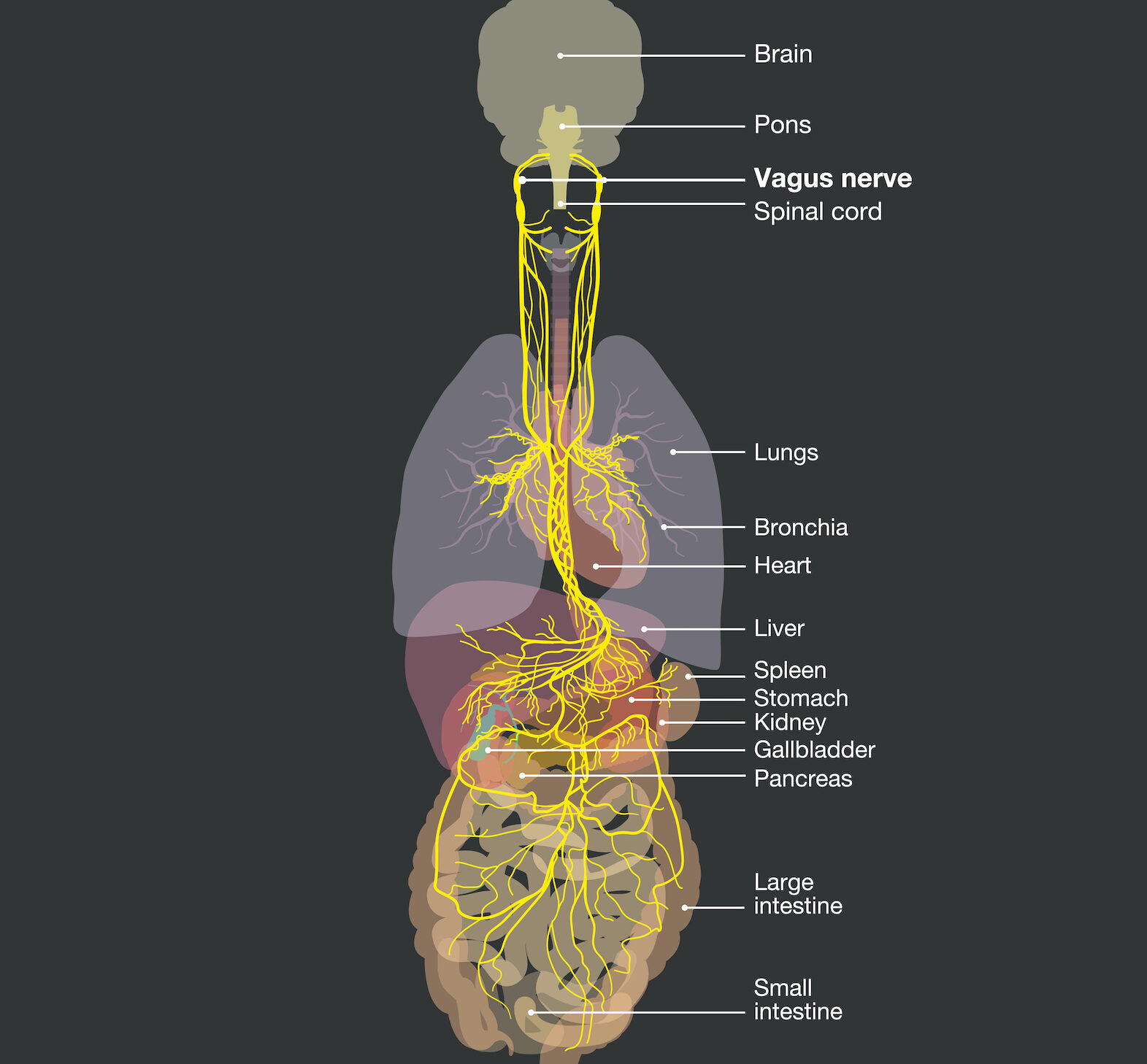
Nerves have a basic job: to transmit signals from one part of the body to another. Since it’s connected to almost every part, the vagus nerve carries the vast majority of that load.
Think of it this way: if the brain is the CPU (central processing unit), then the vagus nerve is the major wire that links to all the other parts of the computer system to make it work.
How the Vagus Nerve Works
Eighty percent of the information transmitted by the VN is afferent information, meaning that the most common direction that information flows in the VN is from the organs of the body to the brain. The remaining 20 percent of the neurons in the VN have an efferent signal, from the brain to the body, leading to specific functions taking place in each cell and organ.
Aha, the Vagus Nerve also observes the 80/20 principle, eh? That’s 80 percent of information carried from the organs to the brain (“afferent neurons”) and 20 percent from the brain to the body (“efferent neurons”).
Upon reaching the nerve endings, the information sent leads to the release of a chemical signal called a neurotransmitter. As for the vagus nerve, the main neurotransmitter is called acetylcholine (ACh), which has a major anti-inflammatory effect on the body.
As we’ll discuss next, managing inflammation is one of the most important functions of the vagus nerve. Dr. Navaz points out that it’s the major inflammatory control system in the body and has far-reaching effects on your health because inflammation is linked to many chronic diseases.
Thus, high levels of inflammation in the body suggest that the vagus nerve is functioning sub-optimally. Not to worry, keep reading and you’ll learn how to optimize it later.
Vagus Nerve Function
The vagus nerve is the conductor of the human body symphony orchestra. It regulates the function of so many different organs and cells in our body, but it can only do so if it is functioning optimally. It must be able to sense and signal correctly to the many organs and cells of the body. Dysfunctional signaling will lead to a lack of harmony in the body, and eventually to a state of dysfunction and disease.
Dr. Navaz compares the body to an orchestra where each of the different instruments has specific parts to play. Then there’s a conductor directing them so every instrument is in harmony with all else, ensuring that nothing is out of tune or off-tempo. That conductor is the vagus nerve, dictating whether the overall sound is music (wellness) or noise (illness).
Let’s have a look at those instruments dictated by the vagus nerve function:
- Sensing Skin of the Ear – allowing us to feel pressure, touch, temperature, and moisture on the central section of each ear. This is clinically relevant because it’s one area for vagus nerve stimulation done with acupuncture.
- Allowing Food to Be Swallowed – managing the process of swallowing each bite and pausing the breathing reflex so that you won’t choke.
- Managing Your Airway and Vocal Chords – to keep your upper airway open when you breathe and makes the sounds audible when you speak. A chronically hoarse voice or an easily fatigued, monotonous voice is a sign of poor vagal tone (signaling capacity).
- Controlling Breathing – relays information to the brain regarding lung expansion levels, as well as oxygen and carbon dioxide levels.
- Controlling Heart Rate – ensuring that the heart rate stays within a comfortable range when the body is not under stress. Without the vagus nerve, our heart would not function near its optimal rate.
- Maintaining Optimal Blood Pressure – relays information to and from the kidneys to help it manage the filtration of the kidney, thus managing the overall blood pressure of the body.
- Controlling the Many Functions of the Liver – how many? Nearly 500 tasks done by the liver. Among which is producing bile and bile salts, as well as transporting bile into the gallbladder and small intestine.
- Activating Gall Bladder Emptying – when fats are being consumed, the vagus nerve signals the liver and gallbladder that bile will be needed for fat digestion.
- Managing Hunger and Satiety – the vagus nerve sends signals to the brain about whether or not the liver has enough fat, protein, and carbohydrates in the body.
- Managing Blood Sugar and Insulin Levels – when activated, the vagus nerve manages the blood sugar levels through the pancreas and maintains insulin sensitivity of the cells in the body. This is linked to switching between the fight-and-flight or rest-and-digest states dictated by the vagus nerve signaling.
- Managing the Release of Digestive Enzymes from the Pancreas – the vagus signals the pancreas to release specific digestive enzymes—proteases, lipases, and amylases—to aid in the breakdown of the macronutrients, allowing for digestion and eventually the proper use of these nutrients by our cells.
- Managing the Activity of the Immune System – think of the immune system like an automobile having gas and brake pedals. The vagus nerve is the one regulating them so we don’t step on both pedals at the same time, or else the machine will break (autoimmune and chronic diseases)
- Managing Inflammation in the Gut – via the neurotransmitter ACh, the vagus nerve balances the parasympathetic and sympathetic activation of the inflammatory response in the gut.
- Relaying Information from the Microbiome – the vagus nerve is the direct link between the brain and the gut microbiome (bacteria). That “gut feel” is possible thanks to the vagus nerve.
- Allowing Us to Create Memories – the chain of communication between the gut and the brain leads to increased neuronal connectivity, and most importantly, the production of memories in the brain.
Whew, that’s a long list… and it’s only a summary!
Vagus Nerve Dysfunction
The results of dysfunctional signaling in the nerve have significantly more damaging and far-reaching effects and can result in the need for diagnosis and treatment with conventional medicine. Keep in mind that vagus nerve tone can be improved and fixed in a vast majority of cases.
We’ve just gone over the many functions of the vagus nerve, I have a feeling you wouldn’t want to see the long list of what could go wrong with a vagus nerve dysfunction, would you?
That’s why we’re only covering the most common dysfunctions (or symptoms) of a suboptimal vagus nerve.
Starting with the most obvious one: dysfunctional breathing.
Notice how are you breathing right now? Put one hand on your belly and one hand on your chest, close your eyes, and take a breath.
Did your belly expand as you took this deep breath or did your shoulders rise to accommodate the expansion of your lungs?
If you breathe through your belly, good job! You’re breathing correctly. But if it’s through your chest, uhmm…
Here’s the thing: when you’re not breathing correctly, you’re not utilizing the muscle for respiration — your diaphragm.
Now, Dr. Navaz tells us that muscle training has a greater effect on the signaling nerve than on the muscle itself. Thus, less muscle activity leads to less efficient signaling of the nerve.
Because our lungs are not fully expanding when we’re not breathing through our diaphragm, the vagus nerve signaling also weakens.
In other words, vagus nerve signaling becomes less efficient as our breathing becomes less effective.
We’ll discuss how we can correct our breathing in the later sections. Keep reading.
Dysfunctional Digestion
An optimal digestive sequence takes approximately 16 to 20 hours to complete, from ingestion of food to release of the waste products. There is quite a bit of variation between people, male and female, healthy and unhealthy, but a transit time shorter than 10 hours is considered too fast, while longer than 24 hours is considered too slow. As vagus nerve activation is responsible for digestive sequencing and peristalsis, dysfunctional digestive rhythm is directly correlated to vagus nerve dysfunction.
In The Awesome Life, I briefly mentioned “mindful eating,” or eating slowly as one of the practical healthy ways to effectively lose weight. To back that up, Dr. Navaz explains the scientific process of what takes place when we eat.
It’s called digestive sequencing.
He says, “All nutrients enter your body through the digestive tract—but only if the sequence of digestion is adhered to.”
The digestive process is very deliberate and slow. So it follows that eating should be done slowly, too. Dr. Navaz puts an emphasis on chewing food well.
The taste of each bite is signaled to the brain to determine how much protein, fat, and carbohydrate is present. Then, the VN signals the stomach, liver, gallbladder, and pancreas to create and pump out the correct amounts of stomach acid, bile, and digestive enzymes.
If we hasten that process, we disrupt the function of the vagus nerve. This causes poor vagus nerve signaling, which leads to a host of digestive issues: diarrhea, constipation, leaky gut, nutrient malabsorption, IBS, or what have you.
To optimize digestive sequencing and vagus signaling to and from the digestive tract, it is necessary to have the vast majority of your meals in a low-stress environment. This means taking time to sit down and eating each meal in a relaxed location.
“Slow food.”
Chronic Inflammation
Chronic inflammation is the most common and obvious sign of ineffective signaling from the vagus nerve.
If we are sending repeated messages of inflammation over a long time, we are essentially training the vagus nerve to stop having its positive anti-inflammatory effect.
Inflammation is the acute response of our immune system to any potential threats and invaders. And which body part is most sensitive to them? Our gut. The majority of our immune and inflammatory cells are housed in the gut, in what’s known as gut-associated lymphatic tissue, or GALT.
Dr. Navaz says the most common source of inflammation they have seen among patients coming to their office is microbiome (gut bacteria) imbalance. This imbalance, if not corrected, triggers the anti-inflammatory cells in the gut for a longer time than necessary. The supposedly acute response becomes chronic and that’s when the problem sets in.
As we are aware, the effect of the vagus nerve is to slow the level of inflammation and keep it in check. If we are sending repeated messages of inflammation over a long time, we are essentially training the vagus nerve to stop having its positive anti-inflammatory effect.
The result of poor anti-inflammatory functioning of the vagus nerve? Autoimmune and chronic conditions. You name it: diabetes, cancer, heart disease, multiple sclerosis, thyroid disorders, psoriasis, rheumatoid arthritis, lupus, celiac disease, and many others.
Okay, I know it’s sounding worse and worse, but hang in there. We’re going to turn it all around in a bit.
Dysfunctional Heart Rate
Electrical signals from the vagus nerve and sympathetic nerves dictate change to the heart rate. The lower your resting heart rate, the stronger your vagus nerve.
The effect of vagus is to slow the heart rate using calming, rhythmic electrical signaling.
Dr. Navaz cites an interesting finding from conducted studies that suggest one’s lifespan is inversely related to resting heart rate, meaning the lower your resting heart rate, the longer you will live.
Thus, we can correlate a longer natural life expectancy with optimal vagus nerve functioning.
During stressful moments, in the fight-or-flight state, the sympathetic nerves activate immediately and the vagus is shut down. The signals from the sympathetic nerves speed up the heart rate by signaling that the muscles of the arms and legs need much more oxygenated blood to take the action needed.
After the stressful event, the sympathetic nerves slowly stop firing and the vagus nerve is able to turn back on.
One sign of a dysfunctional vagus nerve is the inability to quickly normalize the heart rate after a stressful event.
One who’s able to quickly calm their nerves and slow their heart rate has a very strong vagus nerve, while someone who takes longer to come back to their resting rate is likely suffering from dysfunctional vagus nerve tone.
Effects of Chronic Stress on Vagus Nerve
Fight-or-flight vs. rest-and-digest is not like a switch that you can flip to turn a light on or off. It is actually a continuum.
For our bodies to function optimally, we should be on the parasympathetic side of this continuum the vast majority of the time. Approximately 80 percent of the time, we should be activating our vagus nerve and remaining in a relatively parasympathetic state.
Health issues begin to occur when we have trouble switching back from the sympathetic state to the parasympathetic state.
In Healing Code, Dr. Alexander Loyd tells us that the primary underlying cause of disease is stress — physiological stress. And physiological stress happens when the (autonomic) nervous system goes out of balance, which echoes the message of Dr. Navaz.
That is when there’s an imbalance between the sympathetic (fight-or-flight) and parasympathetic (rest-and-digest) nervous systems.
[Read The Polyvagal Theory for an in-depth study of the states of our nervous system and how the vagus nerve relates to them]
If this imbalance becomes chronic, when stress levels remain too high for too long, the parasympathetic system loses the ability to function.
But stress is unavoidable, right? The key is managing it; how we handle stress.
The stressors in our lives, no matter how insignificant they may seem, those “small things” build up and compound over time when not addressed.
If this continues for a long time, we will slowly decrease vagus nerve tone and lean toward vagus nerve dysfunction leading to all sorts of diseases.
Heart Rate Variability
Heart rate variability (HRV) is the gold standard for measuring vagus nerve function. No single test is considered a stronger and more accurate representation of the activity levels of the vagus nerve and vagal tone.
The more active your vagus nerve, the lower your heart rate will be, within an optimal zone, and the more variable the time will be between pumps of your heart.
The higher your heart rate variability, the more likely you are to have a higher level of fitness, cardiovascular health, and vagal tone. High HRV is also one of the best predictors of longevity.
Heart rate variability is the measurement of time, in milliseconds, between successive pumps of the heart—the time from the end of one “lub-dup” to the beginning of the next “lub-dup.”
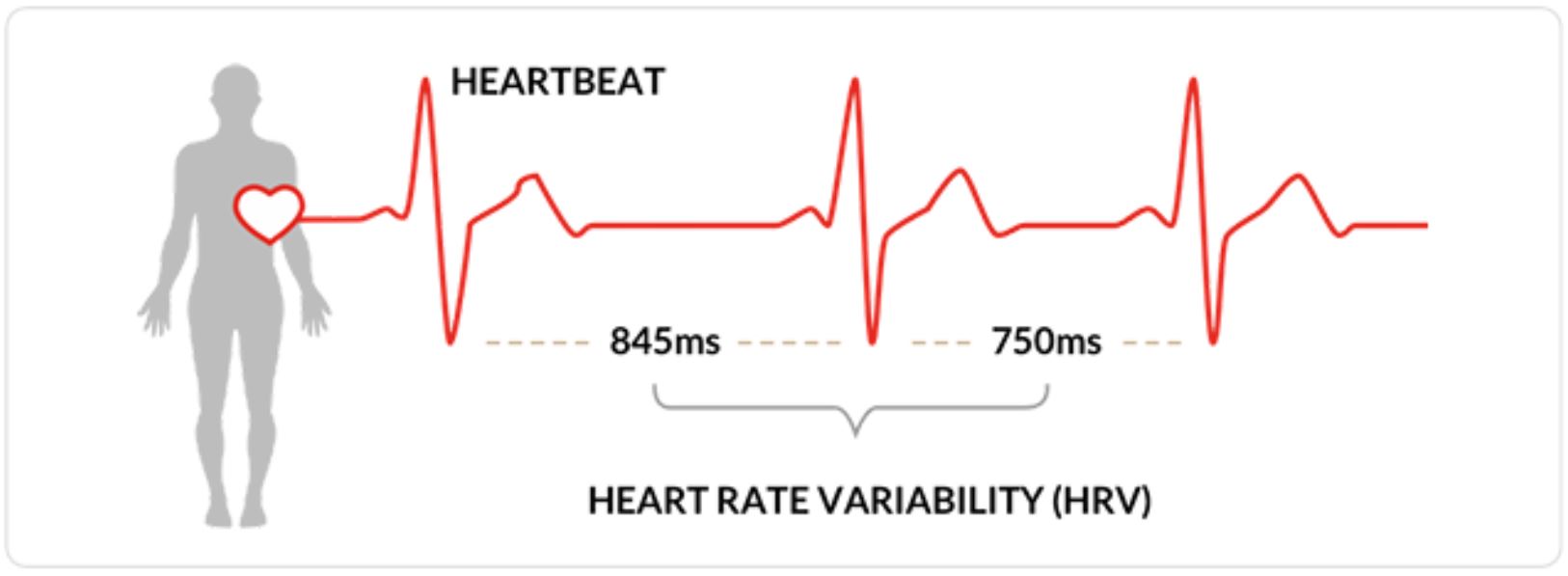
In Becoming Supernatural, Dr. Joe Dizpenza reveals that the heart contains nerves from both branches of the Autonomic Nerve System (ANS). This means that any change in the parasympathetic and sympathetic nervous systems affects the beat-to-beat activity of the heart — the heart rate variability.
“Coherence” is our objective here. We’re aiming for the optimal resting heart rate, which ranges from 50 to 70 bpm. And it’s the signaling of the vagus nerve that’s necessary to slow heart rate and maintain resting heart rate.
Vagus Nerve Stimulation
It is important to remember that the vagus nerve is not simply a parasympathetic signaling nerve: The VN has four separate components, each of which can be stimulated to allow optimal signaling and activation of the other three components.
These components are: (1) skin sensation from the central section of the ear; (2) motor innervation of the pharynx and larynx; (3) parasympathetic innervation of the heart, lungs, and other organs; and (4) afferent vagus neurons that send signals back to the brain through visceral fibers.
Keep these four components in mind as we go through these exercise options.
That’s a lot of jargon, but let’s just put it there for scientific validation as to why the following exercises are effective for vagus nerve stimulation. You’ll find that they are closely tied in with the vagus nerve function and dysfunction we discussed earlier.
BREATHING EXERCISES
The first and most effective way to positively affect your vagus nerve is to learn to breathe correctly. Simply put, rapid, shallow, chest breathing is a sign of stress, which activates the sympathetic branch, while slow, deep, belly breathing is a sign of rest, which activates the vagus nerve.
The Path to Awesomeness Starter Kit got you covered here with the Awareness of the Breath practice. The belly breathing exercise is meant to do exactly what Dr. Navaz tells us — training ourselves to breathe correctly.
Now, how about when we go to sleep? Dr. Navaz shares a life hack that has been effective in improving his breathing patterns — Mouth Taping.
Mouth taping involves putting a piece of tape over your mouth to seal your lips while you are asleep. This essentially forces the airflow to go through your nose while you are asleep.
You can use 3M micropore tape for this purpose.
GET GREAT SLEEP
- Eliminate blue light exposure in the evenings – most electronic devices emit blue wavelength of light that disrupts body signals and hormones for sleep. Here are some tips:
- Enable Night Shift on your Apple devices
- Download the Twilight app on Android devices
- Download f.lux or Iris on your computer (Mac or Windows)
- Use blue-blocking sunglasses if you are watching the television
- Shut off electronics at night – power down your wi-fi routers and put your mobile on silent or flight mode
- Don’t eat or drink too late – your last meal is preferably at least 2 hours before bedtime
- Love your space – organize your bedroom and clean up any mess (for a change, try having crystals or essential oils around)
- Sleeping on your side – A 2008 study by Yang et al. published in Circulation Journal showed that lying on your back is the worst position for HRV levels, while lying on either side showed significant improvement in HRV levels. Most interestingly, sleeping on the right side was found to be the best for vagal modulation.
COLD EXPOSURE
Continuous acute exposure to cold, or cryotherapy, teaches you to regulate your breath, which has an overall positive effect on vagus activation and significant anti-inflammatory effects throughout the body.
Dr. Navaz suggests practicing this during bath time. Take a normal shower, then at the end of the shower, turn the temperature down to as cold as possible and let it hit you on your head and the back of your neck for the final minute of your shower. It will initially be shocking to your system and will change the way you breathe. Then, you practice belly breathing as much as you can. Training yourself to breathe this way through the cold strengthens your vagus nerve functioning.
HUMMING AND CHANTING
When we practice humming and chanting, we are activating and vibrating the laryngeal muscles around our vocal cords and stimulating the vagus nerve to send the signals to and from those muscles.
Chanting the “OM” is one that Dr. Navaz found to be highly effective for vagus nerve stimulation.
ACTIVATING GAG REFLEX
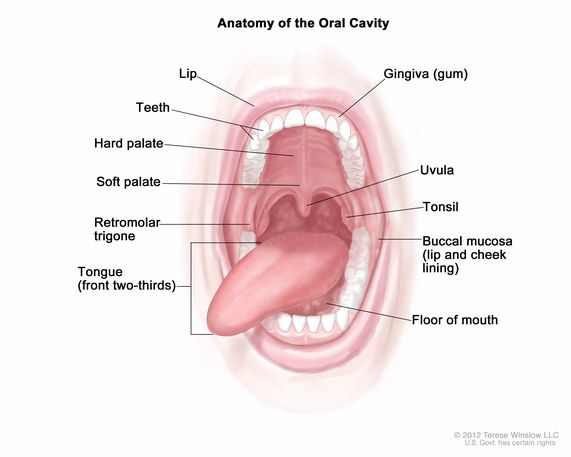
Also known as the pharyngeal reflex, it has similar effects as humming and chanting. The best time to do this is twice per day, while you are brushing your teeth. You can use the toothbrush to touch the soft palate (found in the back of the roof of the mouth) and stimulate this reflex.
GARGLING
Gargling is the act of holding a sip of water in the back of your throat and swishing it around with vigor. It requires activation of the three pharyngeal muscles at the back of the throat, and as such, it is another method of stimulating the vagus nerve through muscle activation. Dr. Navaz suggests doing it rigorously, if you can, to the point that tears are forming in your eyes (a sign that your vagus nerve is firing).
YOGA OR PILATES
These methods exercise optimal voluntary breath regulation while increasing external stressors and teaching you how to control your breath.
MINDFULNESS PRACTICE
Mindfulness practice helps you shift the balance toward the parasympathetic nervous system and allows the vagus nerve to do its job. Paying attention to whatever is happening around you in a calm state engages the vagus nerve and activates it.
MEDITATION
Heart rate variability studies have shown that meditation has significant positive benefits on vagus nerve function because as we meditate, our attention moves toward our breath.
LAUGHTER AND SOCIAL CONNECTEDNESS
Ongoing research repeatedly shows laughter to be very effective in improving mood and heart rate variability. We use our diaphragms when we laugh, and in turn, we exercise our ability to control our breath rate and normalize our breathing patterns. That bellyache laugh is great for the vagus nerve!
Depression, which is often caused by a lack of social interaction, is directly linked to low vagal tone. A 2009 study featured in Health Psychology showed that when patients with symptoms of depression were put into social situations, their mood, heart rate variability, and vagus nerve activity increased.
LISTENING TO MUSIC
A 2010 study by Chuang et al. showed that cancer patients who participated in a 2-hour music therapy session that included singing, listening, learning, and performing music showed significant increases in heart rate variability measures, and thus in vagus nerve and parasympathetic nerve activity.
SMART DIETARY CHOICES
Dr. Navaz recommends opting for green, clean, and lean diets as much as possible. He also says intermittent fasting has been shown to increase HRV, an indication of optimal vagus nerve functioning.
DAILY MOVEMENT OR EXERCISE
Practicing some level of movement, preferably one that helps increase your heart rate by increasing bodily stress levels for a short period of time, helps improve parasympathetic nerve activity. Remember to breathe properly (belly breathing through your nose) when you’re taking breaks to catch your breath.
SUNLIGHT EXPOSURE
Light exposure during the day is directly linked to improved HRV levels. It also regulates your circadian rhythm to help you sleep better at night. The best times to get outside are within 30 minutes of sunrise and within 30 minutes of sunset.
SUPPLEMENTATION
Though supplementation needs vary among individuals, Dr. Navaz has these recommendations that generally work well virtually for everyone (the brands mentioned are what Dr. Navaz uses for his family and his patients):
- Probiotics: MegaSporeBiotic
- Omega-3 Fatty Acids: Ortho Molecular Products and Designs for Health
- 5-HTP for Serotonin (can be used as an effective supplement to allow your body the opportunity to build its own serotonin)
Apart from the list above, Dr. Navaz also lists other options you can consider for vagus nerve stimulation. They are:
- Coffee enemas – for stimulating the ACh receptors in the gut; train the vagus and brain to become highly active and learn to reactivate the gut motility nerves
- Auricular Acupuncture – to increase the flow of information in the auricular branch of the vagus nerve, and thus increase vagus nerve activation
- Massage Therapy and Reflexology – many different techniques of massage have been linked to increases in HRV levels or improved vagal tone; the relaxation helps with parasympathetic activation and sympathetic deactivation
- Visceral Manipulation – done by certified visceral manipulation therapists, it’s a gentle physical manipulation of the organs of the abdomen, thus increasing blood flow to areas that are not functioning optimally
- Chiropractic Care – A 2015 study in the Journal of Chiropractic Medicine showed that spinal manipulation performed by a chiropractor led to significant positive changes in blood pressure and heart rate variability, significantly improving VN activity
Among the methods mentioned above, I’m delighted to offer The Path to Awesomeness Starter Kit, which includes 4 important guided exercises for vagus nerve stimulation, namely:
- Awareness of the Breath – for breathing exercises
- Body Scan with Gratitude – for mindfulness practice and state of gratitude (laughter)
- Heart-Space Meditation – for meditation and listening to music
- Daily AWEffirmations – for chanting affirmations with healing music
Take the step toward your healthy ever after…
Activate your vagus nerve and activate awesomeness in your life now!
ABOUT THE AUTHOR
NAVAZ HABIB is a leading expert in the field of functional medicine and lifestyle interventions using vagus nerve activation. Following his own health-related challenges, he has dedicated his career to addressing the root causes of inflammation, autoimmunity, and metabolic disorders. Trained as a Doctor of Chiropractic and a Certified Functional Medicine Practitioner, Dr. Habib overcame his health challenges using many of the strategies presented in his book. He consults with patients one-on-one at the Living Proof Institute and online through various courses and programs. Navaz Habib currently resides in Toronto, Canada, with his wife Noureen and his daughter Miraal.






